Craniofacial Image Analysis Laboratory (CranIAL)
Overview
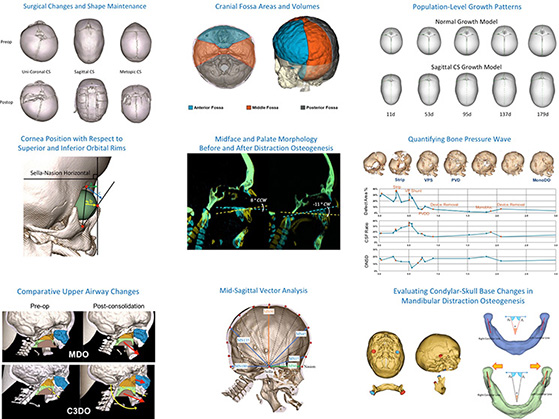
Craniofacial Image Analysis Lab at Seattle Children's Hospital (CranIAL) aims to utilize state-of-the-art image analysis and computer visualization techniques in craniofacial research to improve our understanding of craniofacial disease processes and to assess surgical outcomes. As an interdisciplinary research team, we are dedicated to improving patient care by combining clinical expertise and data-driven research.
CranIAL maintains a growing image database as part of a remote platform that enables a collaborative research environment. In addition to open source tools and off-the-shelf programs, we design and develop custom software to analyze and quantify craniofacial morphologic differences. Lab members gain experience in latest image analysis software and develop critical skills in clinical research.
With a wide range of research projects focusing on different surgical techniques and craniofacial conditions, we have two unifying goals: 1) to develop novel measurements to describe complex or subtle shape differences in craniofacial anatomy, 2) to model the interactions between clinical variables (e.g. patient age, diagnosis, surgical intervention) and changes in craniofacial morphology.
Collaborators
Richard A. Hopper, MD, MS, Chief, Pediatric Plastic and Craniofacial Surgery, Seattle Children's Hospital
Raymond Tse, MD, Pediatric Plastic and Craniofacial Surgery, Seattle Children's Hospital
Srinivas Susarla, MD, DMD, MPH, Pediatric Plastic and Craniofacial Surgery, Seattle Children's Hospital
Murat Maga PhD, Center for Development Biology and Regenerative Medicine, Seattle Children's Research Institute
Sara M. Rolfe, PhD, Center for Development Biology and Regenerative Medicine, Seattle Children's Research Institute
Funding
The Seattle Children's Guild Foundation
Marlys S. Larson Endowed Chair in Pediatric Craniofacial Surgery
Selected Publications
-
- Adidharma W, Mercan E, Purnell C, Birgfeld CB, Lee A, Ellenbogen RG, Hopper RA. Evolution of Cranio-orbital Shape in Non-syndromic, Muenke and Saethre-Chotzen Bilateral Coronal Synostosis: A Case-Control Study of Two-Year Outcomes. Plastic and Reconstructive Surgery. 2021 Jan.
- Susarla SM, Mercan E, Evans K, Egbert MA, Hopper RA. Short-term condylar and glenoid fossa changes in infants with Pierre Robin sequence undergoing mandibular distraction osteogenesis [published online ahead of print, 2020 Aug 17]. Int J Oral Maxillofac Surg. 2020;S0901-5027(20)30258-7. doi:10.1016/j.ijom.2020.07.012
- Nassar AH, Mercan E, Massenburg BB, Lee A, Brown J, Skladman R, Guo Y, Hopper RA. Timing of Ossification of the Anterior Skull Base in Syndromic Synostosis. The Journal of Craniofacial Surgery. 2020 Jul-Aug;31(5):1256-1260. DOI: 10.1097/scs.0000000000006431.
- Mercan E, Hopper RA, Maga AM. Cranial growth in isolated sagittal craniosynostosis compared with normal growth in the first 6 months of age. J Anat. 2020;236(1):105-116. doi:10.1111/joa.13085
- Tse RW, Knight R, Oestreich M, Rosser M, Mercan E. Unilateral Cleft Lip Nasal Deformity: Three-Dimensional Analysis of the Primary Deformity and Longitudinal Changes following Primary Correction of the Nasal Foundation. Plast Reconstr Surg. 2020;145(1):185-199. doi:10.1097/PRS.0000000000006389
- Liu MT, Khechoyan DY, Susarla SM, et al. Evolution of Bandeau Shape, Orbital Morphology, and Craniofacial Twist after Fronto-Orbital Advancement for Isolated Unilateral Coronal Synostosis: A Case-Control Study of 2-Year Outcomes. Plast Reconstr Surg. 2019;143(6):1703-1711.
- Tse RW, Mercan E, Fisher DM, Hopper RA, Birgfeld CB, Gruss JS. Unilateral Cleft Lip Nasal Deformity: Foundation-Based Approach to Primary Rhinoplasty. Plast Reconstr Surg. 2019;144(5):1138-1149. doi:10.1097/PRS.0000000000006182W.
- Susarla SM, Evans KN, Kapadia H, Vasilakou N, Egbert MA, Hopper RA. Distraction Osteogenesis Normalizes Mandibular Body-Symphysis Morphology in Infants With Robin Sequence. J Oral Maxillofac Surg. 2018;76(1):169-179.
- Susarla SM, Vasilakou N, Kapadia H, Egbert M, Hopper RA, Evans KN. Defining mandibular morphology in Robin sequence: A matched case-control study. Am J Med Genet A. 2017;173(7):1831-1838. doi:10.1002/ajmg.a.38248
- Hopper RA, Kapadia H, Morton T. Normalizing facial ratios in apert syndrome patients with Le Fort II midface distraction and simultaneous zygomatic repositioning. Plast Reconstr Surg. 2013;132(1):129-140. doi:10.1097/PRS.0b013e318290fa8a
- Khechoyan D, Schook C, Birgfeld CB, et al. Changes in frontal morphology after single-stage open posterior-middle vault expansion for sagittal craniosynostosis. Plast Reconstr Surg. 2012;129(2):504-516. doi:10.1097/PRS.0b013e31823aec1d
More Information
For current openings and research collaborations, please contact the CranIAL Director, Dr. Ezgi Mercan / Ezgi.Mercan@seattlechildrens.org.